Photography by Hannah KhymychSave this storySave this story
Photography by Hannah KhymychSave this storySave this story
These days, it’s rare to write about plastic surgery without mentioning fat. We’re either losing it (courtesy of GLP-1s), removing it (via liposuction, the top-ranking surgical procedure last year), reusing it (to plump and contour), or, not uncommonly, doing all three in succession—a sort of carefully orchestrated fat shuffle.
Now, plastic surgeons are experimenting with a first-of-its-kind body filler derived from—guess what—fat. Donated human fat, to be exact, which has been procured from cadavers and meticulously processed into a thick injectable called Alloclae. Donor tissue—which includes everything from skin and cartilage to ligaments and heart valves—is frequently used in all fields of medicine, including aesthetics, but for some patients, the idea of receiving “fat from a dead person is still a little macabre,” says Troy Pittman, MD, a board-certified plastic surgeon with practices in Washington, DC, and New York City.
To secure the donor adipose tissue—aka fat—Tiger Aesthetics, the makers of Alloclae, partners with recovery agencies who “work closely with healthcare providers and family members of donors to review the scope of the deceased individual’s donation,” says a representative for Tiger. Some of you may be morally opposed to (or just totally turned by) the idea of using human parts for cosmetic purposes and will choose to avoid Alloclae just as you might forgo Botox (which contains albumin, a protein in human blood) or exosomes (which are commonly sourced from human cells). But this donated fat can also be considered “a natural alternative [to synthetic fillers and implants],” says Dr. Pittman, explaining that the donor tissues are really acting as a scaffolding for your own fat to grow into. “Once your body incorporates the graft, the fat is going to be more yours than the donor’s.”
This isn’t the first time Allure has reported on Alloclae. Back in January, before the product officially launched, I included it in a story about the fat-stimulating shot Renuva. Alloclae isn’t a Renuva knockoff, however. It falls into a separate category all its own. What makes it unique and “potentially groundbreaking,” says Darren Smith, MD, a board-certified plastic surgeon in New York City, is the inclusion of intact, nonliving donor fat cells (and their naturally occurring growth factors), which impart instant volume. Supporting the fat cells in the formula is a proprietary stew of extracellular matrix proteins. These collagens, elastins, and glycoproteins help the donor cells integrate into the body’s own tissue while encouraging innate fat cells and blood vessels to bloom in the area. Renuva, if you recall, is fat cell-free and composed solely of fat-adjacent proteins, which recruit the body’s own fat cells over time.
Designed specifically for the body (the consistency isn’t smooth and fluid enough for the face), Alloclae essentially provides a fat transfer—natural, long-lasting volume—without the hassle, anesthesia, expense, and downtime associated with liposuction. Lipo has forever been a prerequisite for fat grafting—surgeons have to harvest fat from the belly, love handles, thighs, or other areas of excess before processing it and reinjecting it into the body—but it unequivocally adds to the cost and recovery of the procedure and presents its own set of risks, namely contour irregularities (lumps, dents, ripples, and otherwise uneven results). Plus, the thinnest of patients—who are increasing in number with the popularity of GLP-1s—aren’t suitable candidates for liposuction (and therefore fat transfer), since they don’t have much fat to spare. Alloclae not only offers a workaround for these people, but also allows for a non-surgical—and potentially less expensive—fat grafting experience for everyone who might want one. Board-certified plastic surgeon Ashley Gordon, MD, tells me that in her Austin, Texas practice, patients currently pay between $5,000 and $7,000 for 25 ccs of Alloclae, which is enough to “feather in the cleavage” for a modest boost or to hide the edges of breast implants, which can show through the skin of slender patients. Fat grafting done for the same purpose would cost $10,000 or more, because of the time and anesthesia involved with the lipo.
The Science and Safety of Alloclae
“Is it FDA approved?” This is generally the first question we’d urge you to ask about any product you might put in your body. But human tissue-derived materials aren’t vetted in the same way as drugs (like botulinum toxins) and devices (fillers and breast implants). As with Renuva, the FDA regulates Alloclae as a human cell, tissue, and cellular and tissue-based product (HCT/P), which means that while it must meet certain requirements—related to minimizing the risk of disease transmission as well as contamination during manufacturing, for instance—it doesn’t technically have to be “approved” or “cleared” by the FDA, per the agency’s web site.
The Center for Biologics Evaluation and Research, a branch of the FDA, governs these materials, ensuring they meet stringent requirements for safety and sterility. Donors must be thoroughly screened and tested to protect against infectious diseases and microorganisms, for example. (Before gifting any tissues, Alloclae donors “go through an aggressive screening process after they’ve passed away,” explains Sachin M. Shridharani, MD, a board-certified plastic surgeon in New York City and clinical trial investigator for Alloclae.) Additionally, donated tissues must be cleaned and processed in accordance with specific protocols to remove possible contaminants and reduce DNA and other cell components that could provoke an immune reaction or all-out rejection of the fat. “We know that you need to have less than a certain amount of DNA per volume in order to be safe,” notes Dr. Smith, “Alloclae is well below that established standard.”
While FDA requirements for tissue-based products are stringent, the FDA doesn’t demand the same caliber of clinical data—meaning long-term studies on large numbers of real people—as it does when evaluating drugs. When Allure reached out to the FDA for comment on the regulation of Alloclae, a representative for the organization stated that, “The limited information provided on ‘Alloclae’ is not sufficient for us to determine how ‘Alloclae’ is appropriately regulated.”
The published data that currently exists on Alloclae is what’s known as basic science literature—studies involving human cells and mouse models—which essentially shows that the composition of the donor tissue resembles that of native human fat and confirms that any potentially triggering DNA materials have been minimized. The studies also demonstrate that the product does, indeed, integrate into surrounding tissue and promote the growth of new fat cells and blood vessels for a limited time after injection.
When performing a lower body lift on a woman who’d previously had Alloclae injected in the same area, Kamakshi R. Zeidler, MD, a board-certified plastic surgeon in Campbell, California, had the rare experience of seeing the product in the body, three months after it was placed. (Dr. Zeidler is a clinical study investigator for Alloclae.) The Alloclae appeared to be “very well accepted [by her tissues] and it was remarkably soft,” she says.
As for studies involving actual patients, the company says they are “presently supporting five clinical study sites in the U.S. that are treating approximately 50 patients” and that “the study is focused on the application of Alloclae in the hips, more specifically when Alloclae is used to improve the appearance of hip dips.” (These are slight indentations that some people have between their hips and thighs.) While the company does not have results to share at this time, they can say that “several hundred patients have received Alloclae so far this year in both the hip and breast areas and we have received a lot of positive feedback.”
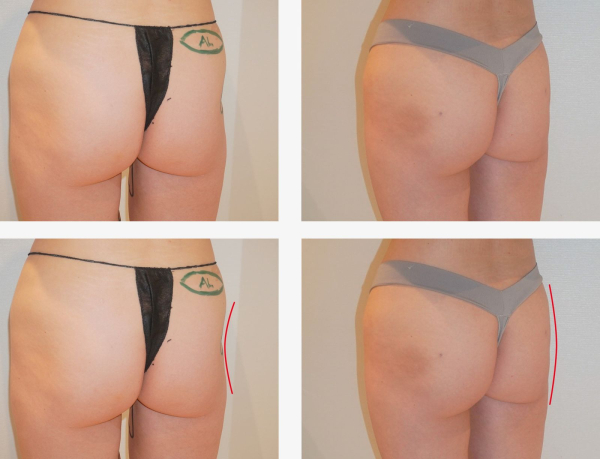
Before (left) and after using Alloclae to correct a “hip dip.” Courtesy of Dr. Darren Smith.
Some doctors have reservations about injecting Alloclae into the breasts specifically, given its relatively short track record. Steven Teitelbaum, MD, a board-certified plastic surgeon in Santa Monica, doesn’t currently stock Alloclae, but says he would consider using it to camouflage divots on the body if he ever encountered patients with this problem. When it comes to the breasts, however, “I’m just very cautious,” he says. “Before trying it out on my patients, I’d want to know more about how it does in the breast: How long does it last? What happens when it dissolves? What are the chances of mammographic changes and palpable irregularities? Is there a way to remove it if it doesn’t look right? I don’t think we can definitely answer these basic questions yet.”
While the uncertainty and lack of human clinical trial data is a sticking point for some, a number of plastic surgeons have adopted the product over the past year, injecting it into patients’ breasts, butts, and hip dips to lend modest volume and round out curves in a conservative—I repeat: conservative—fashion. This is not a means to a massive rear end. “It’s intended for really elegant contouring,” says Dr. Shridharani. He’s also used Alloclae to remedy “devastating deformities” caused by aggressive energy-assisted liposuction. “I see this all the time—thin patients with contour irregularities from liposuction gone awry,” he says. Most “weren’t really lipo candidates, but their surgeons… took a shot at it, piecemealing together what they thought would be enough fat to give a good outcome.”
Before (left) and after correction of liposuction contour deformity (from another surgeon) using Alloclae. Courtesy of Dr. Darren Smith.
When discussing risks with Alloclae patients, plastic surgeons tend to follow a similar script to the one they use for other fat-grafting patients, says Dr. Gordon. In addition to expected side effects, like bruising, swelling, and soreness, possible complications include bleeding, infection, palpable lumps, fat necrosis [tissue death], oil cysts, and underwhelming results. Some surgeons argue that necrosis and cysts may be less of a risk with Alloclae than with a patient’s own fat, since Alloclae doesn’t contain living cells with the potential to die and cause those problems.
A Non-Surgical, Implant-Free Breast Augmentation
In some practices, Alloclae is proving to be a viable alternative to implants. “We see so many women wanting a modest breast enhancement without implants,” says Dr. Pittman—a wish that has historically been granted with fat grafting. But with 75% of these patients, he says, “I can tell within a minute of meeting them that they’re not a candidate for fat transfer, because they’re already very thin.” Before Alloclae, a surgeon in this scenario had two choices: Turn the patient away or attempt to liposuction multiple areas—arms, back, thighs, tummy—and risk traumatizing those body parts in order to get enough fat to make a significant difference. But with Alloclae as an option, “we don’t have to do all that liposuction, we don’t need to use general anesthesia, and we can get a meaningful boost in volume,” says Dr. Zeidler. “We can do Alloclae in the office, under local, and you can drive yourself home after.”
Surgeons inject Alloclae as they would fat, evenly distributing small droplets with a blunt-tip cannula. “I numb the insertion site, and once the cannula is in, the patient may feel pressure, and every once in a while a little zing, but they don’t feel pain,” says Dr. Pittman. When treating the breasts, Dr. Shridharani says he typically makes two two-millimeter incisions (as cannula entry points), one in the breast fold and another at the outer rim of the areola.
The first time Dr. Zeidler used Alloclae, she was treating a woman who’d had a “pretty aggressive explant [breast implant removal] surgery” (done elsewhere) that left her with a flat chest. They started with two rounds of fat transfer, after which the patient desired more volume, but wasn’t up for another round of lipo. She then tried Alloclae and “saw such a meaningful difference from just 50 ccs, which is a much smaller amount than I ever did with fat transfer,” Dr. Zeidler says. Three months later, they did another round of Alloclae and the patient was “ecstatic” with her results. She’s now planning a third session, Dr. Zeidler says, “to get to a nice full C cup.”
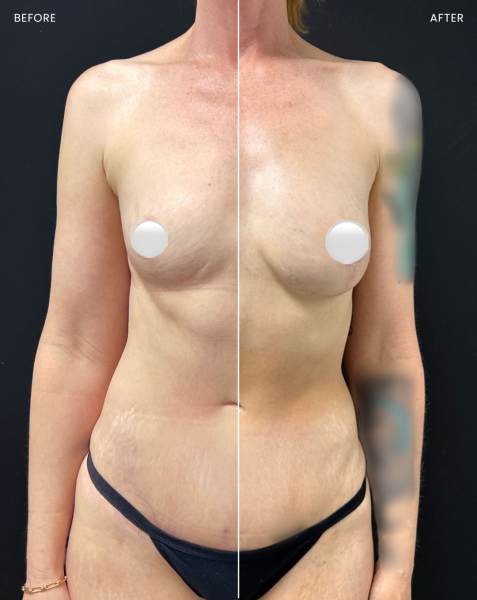
Before (left) and after using Alloclae to make breasts appear fuller. Courtesy of Dr. Kamakshi R. Zeidler.
The size increase achievable with Alloclae depends largely on breast anatomy—in particular, the elasticity of the tissues. When the breasts are very tight, they may not be able to accommodate more than 50 ccs each in a single round, says Dr. Zeidler. But “that’s usually enough to give at least a half-cup boost in volume.” Some women don’t care about bra size so much as “filling out bathing suits,” she adds, and 50 ccs (or even less) of Alloclae can lend nice shape to the tops of the breast to enhance cleavage (though not as effectively as an implant). When patients have bigger breasts or more laxity of their tissues—and, thus, more space to fill—Dr. Zeidler says she can add up to 150 ccs of Alloclae per side for “more than a cup-size increase.” She likes to err on the conservative side, since this is a non-surgical procedure and it’s usually easy enough for patients to come back for a little bit more if needed.
Like Dr. Zeidler, Dr. Shridharani says he can deliver one to two cup sizes with Alloclae, but getting there might require a couple of sessions, a few months apart. It’s important to gradually build volume based on what an individual breast can reasonably hold. The other surgeons I spoke to are, for now, using Alloclae more sparingly in the breasts—25 to 50 ccs per side—usually in conjunction with implants (to veil visible edges or rippling) or after removing implants “to fill out the concavity at the tops of the breasts,” says Dr. Gordon, who’s an advisor to the brand. Wherever Alloclae is used, “it’s important to go slow and be really careful, because this is human tissue,” she says. “It’s not just like a hyaluronic acid filler that we can dissolve with a shot of enzyme.”
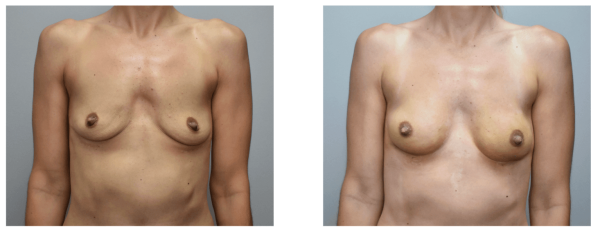
Before (left) and after using Alloclae to enhance the breasts. Courtesy of Dr. Sachin M. Shridharani.
Dr. Shridharani is also seeing “a huge demand” for Alloclae in patients who previously had breast reductions or lifts, and then went on GLP-1s, lost 20 to 30 pounds, and saw their breasts shrink. Assuming their skin quality is still good, and their tissues haven’t stretched, Alloclae can offer a relatively simple solution. (As Allure previously reported, GLP-1 medications are anecdotally linked to impaired collagen production in the skin, primarily because they prompt caloric restriction and nutritional deficiencies.)
I should note that plastic surgeons are somewhat split on the usefulness of Alloclae in GLP-1 patients overall. Dr. Smith says he’s excited to see Alloclae “open up the world of fat transfer to GLP-1 patients who’ve lost volume— maybe not from where they wanted to—and don’t have a lot of fat to donate to the cause.” Likewise, Dr. Shridharani says Alloclae can come in handy in cases where he’d rather not risk creating or exacerbating skin laxity by suctioning what little fat GLP-1 patients have left. Other surgeons see less of a role for Alloclae in this group, especially as a standalone treatment, because these patients often have loose tissue that needs to be tailored and reshaped. In GLP-1 breast patients, “I’m more reliably using implants to create structure,” notes Dr. Zeidler. “ These women generally need breast lifts, as well, to reduce excess skin.” She may use Alloclae after, to fine-tune the results, but it’s not going to save the patient from having surgery, which is ordinarily part of the product’s appeal.
How Alloclae Compares to Implants and Native Fat
The Alloclae aesthetic is distinct from that of breast implants and more akin to that of fat, though not a carbon copy. Implants offer predictable volume—“if we put in a 280 cc implant, we know your breast is going to change by 280 ccs,” says Dr. Pittman—and impart structure, giving the breast a shape to conform to. Fat, on the other hand, is amorphous and creates a more natural effect. Dr. Shridharani explains the difference to patients like this: “Your breast will take on the shape of an implant, be it round or tear-drop, but fat takes on the shape of your breast.” Following fat grafting, “your breast will still look like your breast, only fuller.”
Alloclae falls somewhere in between. Surgeons find it to be thicker and more structural than fat—“it’s giving a lot of lift and shape,” notes Dr. Zeidler—likely due to the way it’s purified and concentrated. When discussing breast augmentation options with patients, Dr. Zeidler puts “soft, fluffy” fat at one end of the spectrum and implants at the other. In the middle is Alloclae: “Compared to fat transfer, Alloclae is providing a more meaningful boost in volume and giving more oomph, cc per cc,” she says. And so far, “it’s looking like the volume we’re putting in is very stable and reliable.”
Dr. Gordon, who’s been using Alloclae for just over a year, says she, too, has found it to be very predictable in terms of long-term gains. “In my experience, the take and retention are really good—like 90% to 100% of what we inject sticks around,” she says. In the first few days after treatment, patients tend to swell. “Some will call me, worried, because it can look bulgy at first, but usually by a week or two, it’s settled down and you can see the correction.”
While studies are being done by the company to quantify Alloclae results at six months and one year, the surgeons I spoke to, who’ve been using it for the past year, have been pleased with the product’s longevity. “It’s almost like what you see on the table is what you get,” says Dr. Shridharani. Since Alloclae can be injected with patients awake, Dr. Shridharani will sometimes have people stand up and look at themselves in the mirror to assess their results. If they like what they see, he might put in a tiny bit more to account for temporary swelling, but otherwise, he says he doesn’t expect the outcome to change very much, because, in his experience, “there’s not a lot of resorption.”
With fat grafting, on the other hand, survival and durability can vary based on myriad factors, including the specific ways in which the fat is collected, handled, processed, and reinjected. In the past, doctors would routinely estimate that about 50% of grafted fat would take. Today, some of the more advanced fat harvesting systems boast retention rates of 75 to 80 percent.
Dr. Pittman, who started using Alloclae in January, says he’s been surprised by how well the product performs, especially compared to fat. “If I were going to graft the upper [portion] of the breast with regular fat, I would need at least 150 ccs of fat for each side, knowing that 50% or 60% may stay and the rest will resorb,” he says. “With Alloclae, I’m using only 50 ccs in each breast to do this, and we don’t see things deflating months later. That’s what’s so phenomenal—the resorption rate seems to be way less than what we see with patients’ own fat.”
At this point, however, Alloclae has been in use for just over a year and “there’s really no data to support what I’m saying here,” Dr. Pittman tells me. “There’s been no real study that I’m aware of looking at overall retention using imaging [to measure volume changes].” He’s very honest with patients about this and careful not to overpromise. “I tell them, fat transfer is unpredictable and we have data,” he says. “Alloclae is unpredictable and we don’t have data.” While anecdotal reports are overwhelmingly positive and Dr. Pittman certainly sees a role for Alloclae, “I’ll feel better when we have published long-term results,” he says. “Something that seems all the rage right now might crash and burn in a year.”
While surgeons can’t conclusively say if Alloclae rivals your own fat, many are cautiously optimistic. Dr. Smith calls the injectable a “super option” for patients who are short on fat, but says he’s still partial to the old-fashioned kind. “All things being equal, I’m going to use native fat every time, simply because it’s living tissue. And with any allogeneic [donor] product, there’s going to be more uncertainty,” he says. Still, other doctors are leaning into Alloclae, especially for small-volume tweaks that may not warrant the heavy-lift of lipo. While I’m reluctant to label anything in the cosmetic realm a “quick fix”—beyond trite, it trivializes medical procedures—Alloclae, some experts insist, could prove to be just that.